More Sleep Improves Overall Health and Wellness

What if I told you more sleep improves overall health and wellness? You read that right- you get to sleep AND get healthier. Easy enough, right? If it’s so easy, how come most of us don’t do it?
When it comes to physical therapy, workout goals, a new diet, or anything else in life, the truth is, until you start optimizing what you do outside of the clinic, the gym, or the kitchen, you’ll never maximize your results.
Research has shown this to be true. One study showed increasing total sleep duration for one week improved performance, reaction time, mood, and fatigue levels. Sleep is an essential part of the recovery process from injury and life stresses alike!
Sleep Improves Recovery
Life is stressful to all of your body’s systems. It’s supposed to be. Recovery trajectory, or the rate at which you recover, is what you can influence with sleep. Getting more sleep will push your recovery trajectory higher while not getting enough sleep moves this downward.
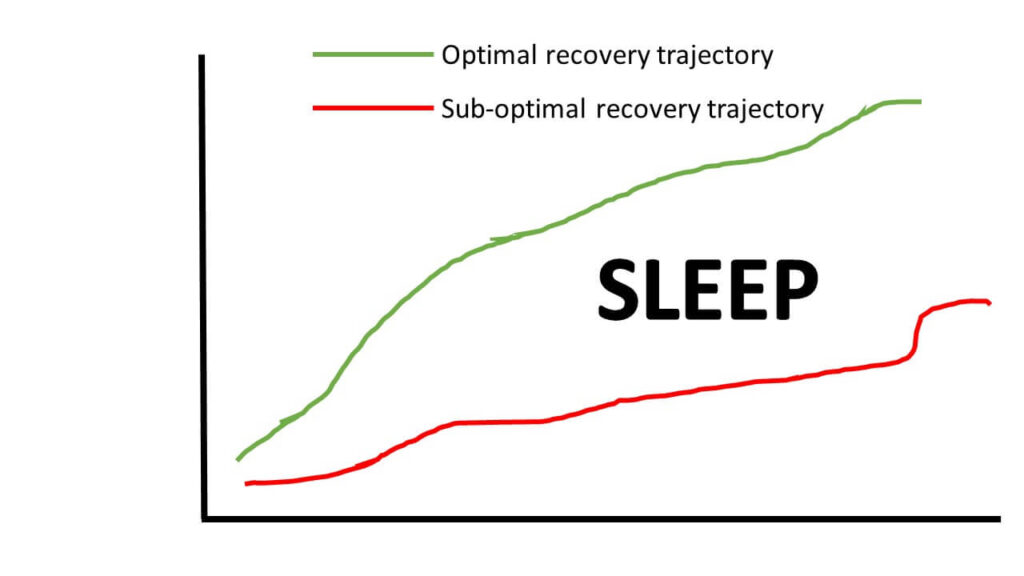
When sleeping, your body is in an anabolic, or building, state. It should go without saying that the more time you spend building and recovering, the better. Being sleep deprived has several potential negative effects. Sleep deprivation can throw off your circadian rhythm, increase heart rate (read: more sleep also has the potential to improve cardiovascular health!), and decrease recovery throughout the day.
On the other hand, less time spent sleeping means more time spent in a catabolic or breaking down, state. This leads to less anabolic (building) hormones that promote recovery and more catabolic (breaking down) hormones such as cortisol that impede it.
Simply put, when you are sleep deprived, your body spends more time breaking down tissue while also not allowing itself to build those tissues back up.
Injury rates increase with fatigue
Sleep rates and injury risk have been studied extensively by the military. There is a clear relationship between sleep deprivation and injury. Soldiers who slept less than 4 hours were nearly 2.5 times more likely to be injured than their counterparts who sleep for at least 8 hours. And even more, risk of injury wasn’t only increased at the extreme end of sleep loss, the rate increased steadily as sleep times dropped below 8 hours.
What does this mean for the rest of us? The less you sleep, the more likely you are to have a musculoskeletal injury.
You are less likely to make healthy choices when tired
Most of us get tired first, then hungry. A 2013 study revealed you don’t just want more food, you want higher-calorie foods when you are sleep deprived. So not only is your body breaking down and resisting repair, but it’s also self-sabotaging. How can anyone be expected to make good choices under these conditions?

With less sleep, your autonomic nervous system (ANS) weakens in its ability to resist impulses (donuts anyone?). With more sleep, your ANS is much better at overriding the desire to reach for less healthy choices- in short, more sleep improves overall health and wellness.
The same can be said for making the decision to work out. Most people don’t skip workouts or home exercise programs when they are well rested. The impulse to skip exercise comes when you are dragging yourself through the day and your fatigued ANS cosigns this bad decision for you.
Strategies to improve sleep hygiene
1. Don’t push an already struggling body
If you’re tired, you may need to adjust the intensity of your work or workout. This isn’t a free pass to skip your workout or home exercise program altogether, but rather the option to scale it to what your body feels like it can do TODAY.
This may be very different from what it did yesterday or what it is capable of tomorrow. Ask your physical therapist which exercises you should do on days when you just don’t have the energy to get through them all.
Adjusting your work to how your body feels is a much better path to recovery than trying to push through a bad night of sleep.
2. Skip the afternoon caffeine
Most of us are convinced we NEED that extra jolt in the afternoon but this could actually be making things worse. This doesn’t mean you can’t have an afternoon latte, simply that you need to make sure it’s early enough in the day to minimize the chance it disrupts your sleep. This is true even if you don’t feel like it affects you. Your body’s ability to eliminate caffeine ranges from 1.5-9.5 hours!
If recovery is your goal, try to plan your caffeine consumption so that it is a far from bedtime as possible. You may not feel the effects of this change immediately, but over time, the quality of your sleep will be improved which ultimately improves your body’s recovery trajectory.
3. Optimize your bedroom for sleep
Given that sleep is so crucial to overall health, your bedroom may be the most important room in your house. It’s important that you set yourself up for success when it comes to good, quality sleep.
For the best chance at getting a good night’s sleep your room should be:
- Dark– Blackout curtains or blinds are inexpensive and easy to find. If you can go to sleep without the TV on, you should (both the light and the noise effect sleep quality).
- Quiet– If you have thin walls and loud neighbors, try a white-noise app on your phone so that adjustments in volume aren’t as jarring.
- Comfortable– Treat yourself to a comfortable bed and bedding. We spend a lot of money on things like phones, laptops, TVs- none of which directly improve health. Work within your budget but take care of your body.
- Cool– Our bodies like to be cool when we sleep. It’s okay to cover up with a good thick blanket, but keeping your room cool while result in a higher quality of sleep.
More sleep is the easiest, most cost-effective way to drive overall health and wellness. If you feel like you are putting in the work but not seeing the results, improving your sleep habits may be just the boost you need to improve recovery and overall performance.
References:
- Jamieson, Joel. “Sleeping Your Way to Fitness.” 8 Weeks Out, 21 Mar. 2021, www.8weeksout.com/2021/03/20/how-to-fix-sleep-improve-fitness-and-recovery/.

She completed a Bachelor of Science degree in Kinesiology with an emphasis in athletic training and a Master of Arts degree in Physical Education with an emphasis in Biomechanics from San Diego State University in 2001 and 2004, respectively.
Prior to physical therapy school, Penny worked as a Certified Athletic Trainer at the University of San Diego, California State University at Northridge, and Butler University where she worked extensively with athletes from the volleyball, baseball, soccer and softball teams.
She is an active member of the APTA, and a credentialed clinical instructor. She has presented at national meetings on Kinesiophobia in Outpatient Physical Therapy, Differential Diagnosis of Ankylosing Spondylitis, Transient Osteonecrosis of the Femur in an Active Female, and Tibial Plafond Fracture in a High-level Distance Runner. She has also published on topics including returning to sports after anterior cruciate ligament reconstruction and fear of movement/re-injury across the spectrum of outpatient physical therapy diagnoses.
Penny has extensive continuing education training in running gait analysis, biomechanics of the shoulder in overhead athletes, strength training for runners and youth athletes, post-surgical rehabilitation and return to sport testing protocols, and training the female athlete.
Dr. Penny Goldberg, PT ATC earned her doctorate in Physical Therapy from the University of Saint Augustine in 2012 and completed an American Physical Therapy Association (APTA) credentialed sports residency at the University of Florida in 2014. At UF she provided physical therapy services for varsity athletes from all sports. Penny is a Board Certified Sports Clinical Specialist.
She completed a Bachelor of Science degree in Kinesiology with an emphasis in athletic training and a Master of Arts degree in Physical Education with an emphasis in Biomechanics from San Diego State University in 2001 and 2004, respectively.
Prior to physical therapy school, Penny worked as a Certified Athletic Trainer at the University of San Diego, California State University at Northridge, and Butler University where she worked extensively with athletes from the volleyball, baseball, soccer and softball teams.
She is an active member of the APTA, and a credentialed clinical instructor. She has presented at national meetings on Kinesiophobia in Outpatient Physical Therapy, Differential Diagnosis of Ankylosing Spondylitis, Transient Osteonecrosis of the Femur in an Active Female, and Tibial Plafond Fracture in a High-level Distance Runner. She has also published on topics including returning to sports after anterior cruciate ligament reconstruction and fear of movement/re-injury across the spectrum of outpatient physical therapy diagnoses.
Penny has extensive continuing education training in running gait analysis, biomechanics of the shoulder in overhead athletes, strength training for runners and youth athletes, post-surgical rehabilitation and return to sport testing protocols, and training the female athlete.



